The COVID-19 pandemic amounted to a cumulative $1.44 billion daily revenue loss for hospitals between March and mid-April , according to reports from healthcare advocacy and advisory groups.
An
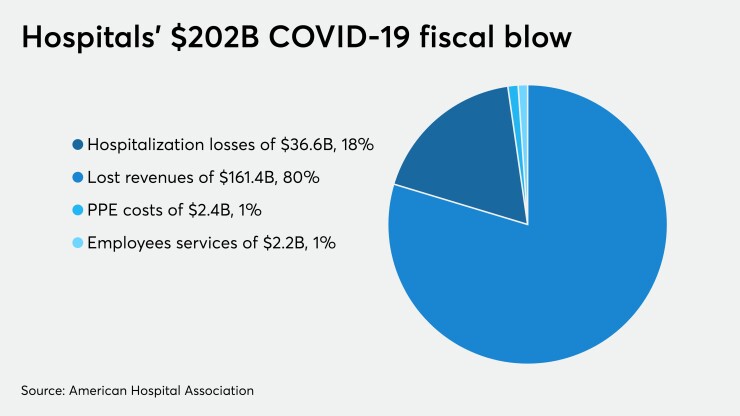
Expenses also include hospitals’ coverage of daycare, transportation, and temporary housing for some employees. The numbers don’t include other expenses, such as increased personnel and drug expenses, which are still being assessed.
“Hospitals will likely continue to see lower service use while treating COVID-19 patients beyond June 30, which would result in continued financial pressures,” the AHA said. “The totality of these costs combined with the uncertainty of the pandemic’s duration is certain to imperil hospital finances.”
A series of federal relief packages has provided relief for hospitals, including direct aid of $100 billion from the Coronavirus Aid, Relief, and Economic Security Act that also speeds up Medicare reimbursements. The latest aid package earmarks another $75 billion to reimburse hospitals, systems and providers for expenses and lost revenues.
“While we appreciate the support and resources from Congress and the Administration, many hospitals are still on the brink,” AHA president Rick Pollack said. “We need further support and resources to ensure that we can continue to deliver the critical care that our patients and communities are depending on while also ensuring that we are prepared for the continuing challenges we face from this pandemic as well as other potential emergencies.”
The group also cautioned the estimates through June could change as elective surgeries and other diagnostic tests and procedures are coming back on line at varying speeds. In some states, hospitals have resumed such services while in others the guidelines are still being laid out. The federal government recommended a halt to such services in March to preserve hospital beds for COVID-19 patients and some states mandated a stoppage.
The aid so far is not enough, as many hospitals suffered fiscal strain before the pandemic, the AHA said citing a Congressional Budget Office projection that between 40% and 50% of hospitals could see negative margins by 2025. Fund distribution and timeliness of payments also concern the group.
Estimates of the cost of treatment and reimbursement vary greatly. The Kaiser Family Foundation estimates the cost of treating a patient with COVID-19 could be more than $20,000 and over $88,000 for patients that require ventilator support, while a FAIR Health estimate puts the average cost of treating patients with commercial coverage at $38,221, the AHA said.
“At the same time, experts anticipate that millions of Americans could become uninsured given the spike in unemployment. The number of people without insurance could increase to over 40 million,” the AHA warned. “These coverage losses put families at financial risk and increase uncompensated care at hospitals. Hospitals have already seen some of the effects manifest. Bad debt and charity care increased 13% over the previous year in March,” according to data from the advisory firm Kaufman Hall.
A
That equates to a $1.44 billion net daily revenue hit for hospitals with more than 100 beds, according to a review of data gathered by Crowe, an accounting, consulting and technology firm. The assessment did not include hospitals in New York City and San Francisco.
"Hospitals and governments prepared for a surge in patient volume to treat those infected with the novel coronavirus," said Brian Sanderson, a managing principal of healthcare services at Crowe. "However, any possible surges that might have been expected due to COVID-19 patient volume appear to be dramatically offset by a significant decline in volume in all other areas."
The impact covers both procedures that ground to a halt and hospital visits that otherwise slowed. Inpatient admissions were running more than 30% below norms compared to January 2020, with emergency room visits down 40%. Observation services were 47% lower than usual. Outpatient ancillary services fell 62%. And outpatient surgery volume dropped 71%.
In California, overall patient volume was down 50%. Florida saw a 47% drop and Texas took a 56% hit, while Illinois saw a 59% drop.
"Despite government monetary relief and supply assistance, the economic effects of March and April 2020 will affect the operations of our healthcare system long after the curve flattens or dissipates,” Sanderson said.
Hospitals, initially in triage mode, focused on liquidity, tapping or establishing new lines of credits and putting off capital expenses. Hospitals have responded to the fiscal wounds through a mix of measures, with some turning to credit lines or furloughing employees. The rating agencies hold a negative view of the sector and some hospitals have already received credit warnings.











