Texas lost another rural hospital when Hamlin Memorial Hospital near Abilene closed July 31.
The hospital in the West Texas county of Jones was built and managed by the Hamlin Hospital District, whose last bonds were paid off 12 years ago. The town of 2,018 has lost population since the 2010 census.
"Over the past many years inpatient utilization has decreased to the point that there are many days that there is no one in the hospital," the hospital said in announcing the closing. "After an in-depth study of all departments in the hospital, income vs. expenses, it became very evident that Medicare, Medicaid, and most private insurance reimbursements did not come close to covering continually rising expenses. A declining tax base and tax payment delinquencies have also contributed to the financial hardships."
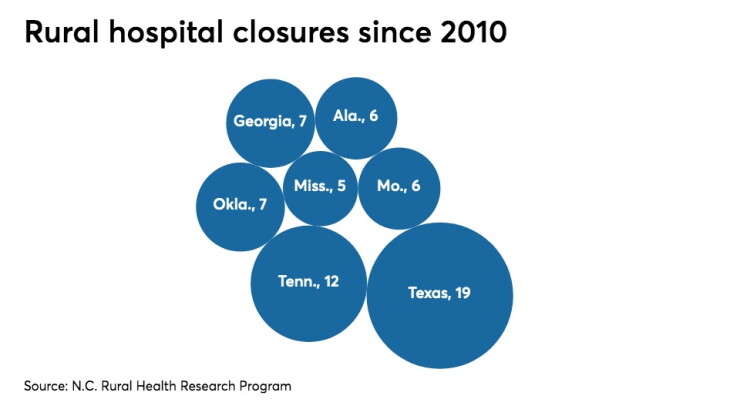
In less than a decade, 19 hospitals in Texas have closed, the most of any state, according to the North Carolina Rural Health Research
Statewide, Texas has about 160 rural hospitals. The Hamlin closure comes one year after the Stamford Healthcare System, 20 miles away, announced that it was ending hospital inpatient care and emergency room services, blaming a drop in patient numbers and a failure to meet Medicare requirements. A hospital in Anson, 17 miles away, is the closest to Hamlin.
Hamlin has had a hospital serving the town since 1948. The hospital district was created 25 years later. A 25-bed Hamlin hospital that cost $1.8 million opened April 27, 1980. A subsequent fundraising drive netted $140,000 to buy equipment for the facility.
Patricia Barnett, president of the hospital district's board of directors, said in a Facebook post that the walk-in clinic would remain in operation.
“Today marks the end of an era of healthcare for us,” she said. “Our beloved Hamlin Memorial Hospital will close its doors tonight at midnight. As I walked through the halls of our hospital for the last time today, so many memories flooded through my mind. I can say with all certainty that we did our job well, with love, dedication and pride for the patients that graced our doorways."
Studies show that more than 70% of the rural hospital closures came in states that refused to expand Medicaid coverage to the working poor under the 2010 Affordable Care Act.
In December, a Texas federal judge ruled that the ACA must be abolished as unconstitutional. The Fifth U.S. Circuit Court of Appeals in New Orleans is considering whether to uphold the ruling, which would eliminate health insurance coverage for 20 million Americans.
In July, a three-judge panel of federal appeals judges aggressively questioned whether the health-care law known informally as Obamacare should be allowed to survive.
Two Republican appointees on the three-judge panel frequently interrupted attorneys to question whether the Affordable Care Act’s individual mandate is unconstitutional.
A ruling by the Fifth Circuit Court is expected to be appealed to the U.S. Supreme Court.
In 2019, 46% of rural hospitals operate at a loss, compared to 44% in 2018 and 40% in 2017, according to the National Rural Hospital Association. Due to financial strains, nearly 700 rural hospitals are financially vulnerable and at high risk of closure, the NRHA says.
“Continued cuts to rural providers are creating a hospital closure crisis in rural America, jeopardizing millions of rural patients’ access to medical care and devastating the already fragile rural economy,” according to the National Rural Health Association. “Currently one in three rural hospitals is in financial risk. At the current rate of closure, 25% of all rural hospitals will close within less than a decade.”
Voters in rural counties have proven reluctant to support local hospitals with their property taxes. After a loss of $6.2 million, St. Mark Medical Center serving Fayette and Lee counties, asked voters this year for permission to tax property owners up to 25 cents per $100 in property value to settle the 2017 debt. The proposal was defeated with 80% opposed. The hospital continues to operate, however.
Voters in the East Texas town of Crockett rejected a tax levy after the hospital closed in 2017. In 2015 voters allowed Bowie Memorial Hospital to close after rejecting tax support. Bosque County voters rejected hospital funding in 2010.
The 2019 Texas Legislature approved $16 million more in Medicaid funding for labor and delivery services at rural hospitals over the next two years, or about $500 more per delivery. However, lawmakers also added a burden to publicly funded hospital districts with reforms designed to lower property taxes.
About 60 million people live in parts of the nation considered rural or frontier, according to the National Rural Healthcare Association, and about 75% of rural counties have been designated as medically underserved areas.
Telehealth – the practice of medicine over a long-distance network or the internet can increase access to physicians, specialists, and other healthcare services for patients in rural, frontier, and underserved areas, the association said.
“However, there are many barriers to wide adoption of telehealth in rural America,” a policy
Telemedicine adoption rates vary significantly by state, researchers say. Alaska has the highest rate in the country with an adoption rate of 75%. But, states frequently require providers to be licensed in the same state as the patient they are treating, they say.
“One large barrier to the adoption of telehealth is broadband infrastructure,” the study says. “Many rural, frontier and underserved areas do not have access to appropriate broadband to allow for the use of telehealth. According to the Federal Communications Commission, 34 million Americans still lack access to adequate broadband.”











