Not-for-profit hospitals need additional federal relief to avoid deep COVID-19 fiscal wounds that could leave half of the sector operating in the red by the end of the year, financial advisory firm KaufmanHall warns in a report.
The American Hospital Association sought to draw attention to the report — “The Effect of COVID-19 on Hospital Financial Health” — by publishing it on its website and holding a conference with KaufmanHall managing director and founding partner Ken Kaufman along with hospital officials.
They join the chorus of local and state governments, higher education, business and other advocacy groups in lobbying efforts as work on the next stimulus/relief package heated up this week. Four packages have been approved so far, providing $3.6 trillion in various forms of support.
“Our forecast shows that, without further government support, margins could sink to negative 7% in the second half of 2020. This is an unsustainable level for America’s hospitals,
Hospital margins took their deepest blow in April as hospitals experienced a full month of rising costs associated with staffing and equipment costs to deal with the pandemic while elective procedures ground to a halt, often by order of state governors. May numbers improved slightly, as hospitals recorded federal relief on their balance sheets and revenue picked up from resumption of elective procedures and surgeries.
Without more aid, the report warns, the median hospital margin could land at a negative 1% to negative 11% for the full year, depending on the course of the coronavirus. The fiscal wounds are difficult to accurately predict because future surges, another halt to elective surgeries and procedures and lackluster volumes based on patient decision-making will influence the numbers.
“For any organization, a positive operating margin is essential for long-term survival,” the report notes. "Few organizations can maintain themselves for an extended period when total expenses are greater than total revenues. For hospitals, positive financial margins allow them to invest in new facilities, treatments, and technologies to better care for patients, and to build reserves to meet unexpected expenses or revenue shortfall.”
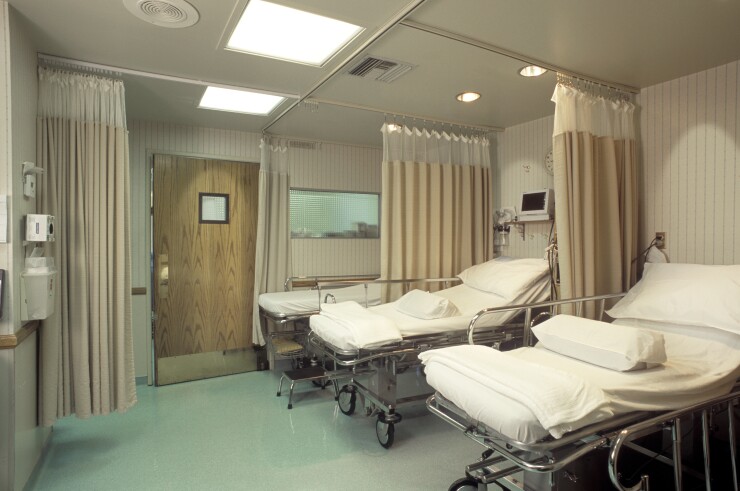
Without the infusion of $175 billion in aid, including $100 billion in direct funding from the CARES Act signed March 27, margins would have fallen to negative 15% in the second quarter. With the funds, margins will still land at negative 4% for the second quarter. That compares to the median of positive 3.5% before the COVID-19 pandemic.
About 45% of all hospitals recorded an operational loss for the second quarter and even though revenue is picking up with the resumption of elective procedures and surgeries, the report warns 51% may still be operating in the red in the fourth quarter without any further support.
“Heading into the COVID-19 crisis, the financial health of many hospitals and health systems was challenged, with many operating in the red,” AHA President Rick Pollack said. “This pandemic is the greatest financial threat in history for hospitals and health systems and is a serious obstacle to keeping the doors open for many.”
The AHA had previously put the potential toll of losses at $120.5 billion for the second half of the year, due primarily to lower patient volumes. That’s on top of a $202.6 billion blow between March and June.
The AHA, American Medical Association, and American Nurses Association on Wednesday sent a letter to Senate Leader Mitch McConnell, R-Ky., and Minority Leader Chuck Schumer, D-N.Y., urging the allocation of at least $100 billion in direct emergency aid. They warn the ability for some hospitals to remain afloat is at stake.
“Front line health care providers are experiencing significant financial losses due to the decrease of inpatient and outpatient services. In some communities where COVID-19 is spiking, hospitals again have stopped providing non-essential surgeries to ensure there is increased capacity for COVID-19 patients, resulting in additional significant financial loss,” the letter warned.
As bad as the numbers look so far this year, Fitch Ratings said they could have been worse. The numbers are not “as bad” as “what we were thinking just a quarter ago," Fitch senior director in public finance healthcare Kevin Holloran said on a healthcare webinar Fitch hosted last week.
Holloran attributed that to the federal aid and hospitals’ quick action to manage costs. The equities market has also recovered from deep drops early in the pandemic and that also helped hospitals improve metrics, allowing many to avoid covenant violations.
Some downgrades occurred, but affirmations were more frequent with little in the way of upgrades.
The pandemic may result in an acceleration of consolidation and partnerships, Holloran said. Mergers and acquisitions have been steady in recent years as the sector deals with a changing federal and payor landscape and hospitals and systems joining forces allows for a greater leveraging of their size to manage costs. Smaller, independent hospitals have sought partnerships or unions just to stay afloat.
Holloran predicted increased activity on all fronts from large systems merging with other large systems to systems picking up independent hospitals. He also sees hospitals forming or cementing partnerships as the pandemic has shone a light on the benefits of collaboration and affiliations.