Officials from New York City Health + Hospitals are examining the effects of COVID-19 preparation on its already strained bottom line.
The largest municipal healthcare system in the U.S. and the city’s safety-net system, H+H operates 11 acute-care facilities, five skilled nursing facilities and dozens of community-based health clinics.
Speaking at a City Council hospitals committee budget hearing, H+H chief financial officer John Ulberg said the system has already spent $2.1 million through Monday afternoon on virus preparation.
“That number will clearly go up as the virus progresses, but our direction to our clinicians is to battle the problem and we’ll figure out the money later," Ulberg said. “It’s important that we have accurate accounting so that when federal funds or state dollars or whatever dollars become available to us, we have the appropriate accounting.”
Last week, Mayor Bill de Blasio's budget director,
The federal government last week authorized $8.3 billion in emergency funding for COVID-19, with $35 million earmarked for New York State.
Health + Hospitals has worked amid disasters such as Sept. 11 and Hurricane Sandy.
H+H has long been a strain on the city’s operating and capital budgets. Projected cuts from the state as it seeks to close its own gaps related to Medicaid and uncertainty regarding federal funding loom large.
“We certainly don’t need additional headwinds given the challenging and evolving situation we’re dealing with,” said senior vice president Matthew Siegler.
Gov. Andrew Cuomo has reconvened his 21-member Medicaid redesign team, which to the chagrin of some advocates lacks city and H+H representation. The panel is looking to identify $2.5 billion in statewide savings.
While the impact on H+H remains unclear, the proposed state budget presentation contains language permitting the governor to implement across-the-board cuts should the $2.5 billion in savings not materialize by April 1.
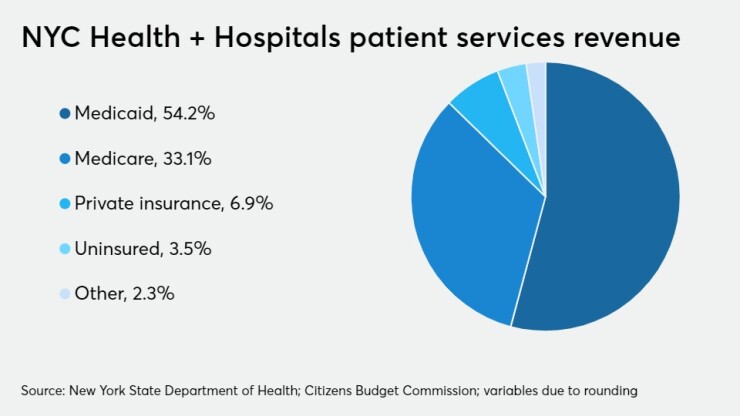
H+H remains the city’s largest healthcare provider to Medicaid patients and people without health insurance. The system relies heavily on Medicaid revenues — $2.2 billion in fiscal 2020 — while payments under the Disproportional Share Hospital under supplemental Medicaid and city support in FY20 account for $2.5 billion and $899 million, respectively.
A December report by the watchdog
Without revenue enhancements and cost-cutting, H+H is projected to have operating losses of $1.3 billion to $1.9 billion over four years.
De Blasio in 2016 began a transformation plan called “One New York: Health Care for our Neighborhoods.”
H+H reported just under $900 million in outside revenue in fiscal year 2020, including $773 million in city funding, $110 million in intracity funding, $2 million in city noncash funding, and $13 million in federal funding.
For fiscal 2021, it reports $1.058 billion in outside revenue, including $970 million in city funding, $85 million in intracity funding, and $2 million in city non-cash funding, with no federal funds recorded.
According to Siegler, H+H closed with first half of fiscal 2020 with a “strong” cash balance of $790 million.
The system, he said, is generating more revenue through more efficient billing of insurance companies; improving its outpatient coding and physician billing practices; and signing more patients for insurance. “We’ve seen a 20% increase in insurance applications,” he said.
“We’re negotiating with insurance companies for fair fates for the services they provide, as well as settling for back payments they owe us,” Siegler added. “We’re providing more specialized clinical services with higher reimbursement rates while continuing to expand access to primary care for all.”